Fighting Childhood Pneumonia
Turning a Medical Crisis into an Engineering Challenge to Save Lives
Pneumonia is the number-one infectious cause of death for children under age five worldwide. According to UNICEF, pneumonia claimed the lives of more than 880,000 children in 2016 — most of whom were less than two years old. Treatment for pneumonia is not the primary issue as readily available antibiotics are highly successful. Misdiagnosis is the main challenge.
In hard-hit areas such as sub-Saharan Africa, misdiagnosis stems from the combination of limited numbers of medical professionals and clinics that often lack diagnostic tools. In fact, many remote clinics do not even have a computer, let alone an x-ray machine that can definitively diagnose pneumonia.
Further complicating the issue, malaria shares many symptoms with pneumonia, including fever and chills. In the areas hardest hit by childhood pneumonia, the population continues to struggle with both diseases. Despite similar symptoms, treatments for malaria and pneumonia are quite different. Pneumonia, an infection of the lungs, is treated with antibiotics, while antimalarial drugs eliminate the malaria-causing parasite from the patient’s blood. With such different treatments, a misdiagnosis often proves deadly.

Data Source: UNICEF
Diagnosing Pneumonia
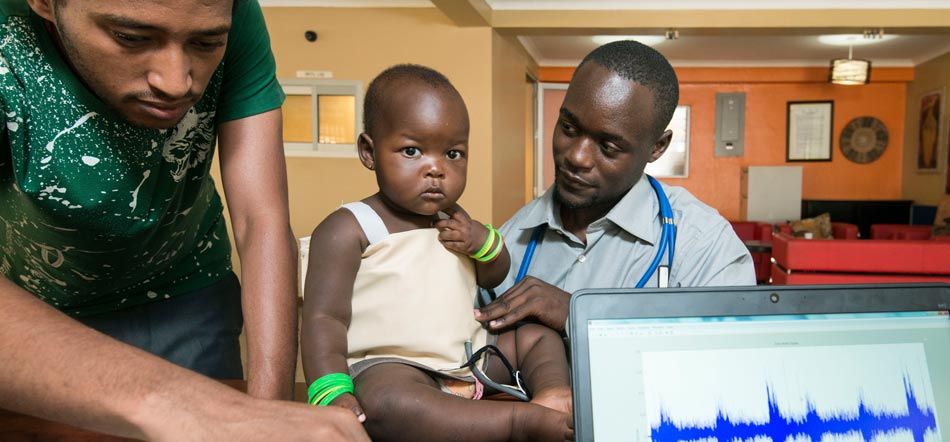
When a doctor is available, the first steps in diagnosing pneumonia are to measure respiration rate and use a stethoscope and listen for the telltale crackle sounds in the patient’s lungs. In Uganda, there are fewer than two doctors for every 20,000 people, according to the World Bank Group. (By comparison, Germany has 84 doctors per 20,000 people.) Given the low numbers, that critical first step is not often feasible.
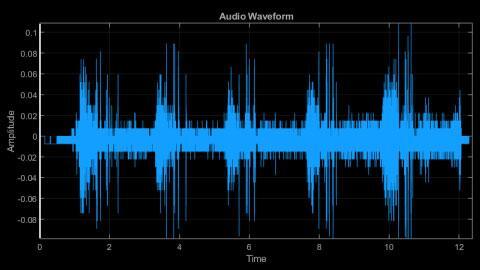
Here is what pneumonia sounds like:
Audio Source: thesimtech.com
Understanding the impact of so few doctors in the region, a team of recent engineering graduates in Uganda set out to find a way to help their community prevent pneumonia deaths. They realized nothing could completely replace the effectiveness of a qualified doctor with a stethoscope, so they stopped looking at the challenge as a medical problem and instead called upon their engineering and data science skills to approach the issue as an engineering problem.
Brian Turyabagye and two colleagues from Makerere University in Kampala, Olivia Koburongo and Besufekad Shifferaw, founded Mama-Ope in 2016. Meaning “mother’s hope,” Mama-Ope took its initial inspiration from Koburongo, who lost her grandmother to a misdiagnosed case of pneumonia. Upon learning the misdiagnosis problem is more prevalent among children, they focused their efforts on saving these young lives.
According to Turyabagye, attacking this from an engineering perspective revealed very solvable aspects to the problem.

Mama-Ope Founders: Olivia Koburongo (left), Brian Turyabagye (center), Besufekad Shifferaw (right)
Image Credit: RAEng/Brett Eloff
"Research shows that pneumonia can be identified by four major vital signs: the breathing rate, temperature, the lungs’ sounds, and the oxygen saturation in the body. It also shows that if you can capture accurately three out of four of these leading signs, you’re able to accurately predict the state of pneumonia in a child.”
Child wearing prototype Mama-Ope jacket
Image Credit: RAEng/Brett Eloff
Converting Symptoms to Data
Turning the medical issue into an engineering problem required turning the symptoms into data. The major vital signs of temperature and breathing rate were relatively straightforward to measure. Quantifying the lung sounds was a bigger challenge. The team needed to capture the lung sounds from multiple locations on the child’s torso without a stethoscope, so they designed a wearable medical device: a smart jacket. The group’s Mama-Ope smart jacket prototype has five microphones effectively serving as a wearable stethoscope.
Physicians can tell a lot from listening to just the right spot on a patient’s chest but unfortunately, the Mama-Ope jacket doesn’t have the luxury of finding that spot. It must settle for a good-enough spot. This is where the jacket’s form factor comes in; the microphones are strategically located in the jacket, so they are correctly positioned on the patient as soon as the jacket is donned. But each patient is different, and a doctor would shift the stethoscope around if the sound isn’t clear enough. Collecting sound data from five microphones helps ensure enough sound data is recorded to make up for any differences in recording quality for a given patient.
Once the data is collected, diagnosing pneumonia — including detecting the progress of the disease — becomes a data science challenge. The problem is fundamentally one of audio processing. What are the characteristic sounds that would come from a pneumonia-infected child wearing the Mama-Ope jacket?
The Mama-Ope team programmed a signal-processing algorithm to provide the best diagnostic insight available from the audio recordings. The goal: Determine when the distinctive crackle sound of pneumonia was recorded. Heuristically, the distinctive lung sounds include wheezing and crackling. The Mama-Ope algorithm, Turyabagye says, processes each of the five microphone inputs separately to determine if the crackle is present.
“Each part of the lung has its own significant characteristics. So, signal processing for each microphone can be fine-tuned to suit the sonic profile of a pneumonia signal for that specific region of a child’s lung.”

Signal processing and wavelet analysis help find distinctive features in the sound data.
The team collected clinical data and, with the help of medical professionals, labeled the recordings of healthy patients and those with known cases of pneumonia. This data was used to create and test their signal-processing algorithms.
To help develop these algorithms, Turyabagye sent sound files to Kirthi Devleker at MathWorks—sound files that corresponded to confirmed cases of pneumonia. Devleker, a technical expert in signal processing and wavelets, said:
“We wanted to take a step back and see what distinctive patterns were present throughout all the signals. We found some features for the crackle sound, and they are very consistent from a signal-processing perspective.”
Turyabagye and Devleker analyzed and explored the signals in MATLAB using signal processing and wavelet techniques. They found distinctive features that, through the use of machine learning, can aid in diagnosis.
“Once you identify and extract the features and pair it with a machine learning algorithm, you make the task of classification very easy. The data can be used to train a machine learning algorithm, which can predict the cases where pneumonia is present.”
The jacket is designed to be used at remote clinics and schools. Even locations without medical personnel or a computer can use the jacket for a speedy diagnosis. The jacket connects to a mobile phone app via Bluetooth which records and analyzes the collected data. It then sends the results to a health care professional, so he or she can make an informed diagnosis without requiring an in-person examination of the child.
Next Steps
Turyabagye says their prototype smart jacket only requires a child to wear it for about three minutes, so even a single Mama-Ope jacket in a clinic or school could result in many fast and accurate diagnoses where doctors are unavailable.
With the working prototype complete, Mama-Ope’s next challenge is to clear regulatory hurdles in Uganda, where Turyabagye says the company will first be rolling out its technology. Beyond Uganda, the company plans to expand its rollout to nearby countries, including Kenya, Tanzania, Ethiopia, and Nigeria.
He says UNICEF has already expressed interest in helping Mama-Ope bring its technology to schools, hospitals, and clinics in the region. Then perhaps UNICEF, too, might one day report childhood pneumonia deaths were reduced with the help of a smart jacket and a fair amount of Ope.

A doctor adjusts the sensor-laden Mama-Ope jacket on a child.
Image Credit: RAEng/Brett Eloff
Read Other Stories
AI
Cyborg Drummer and AI Team Create Music That’s Not Humanly Possible
Designing a Robotic Prosthetic for a Professional Drummer